Prostate Cancer
Tests involved with prostate cancer treatment
What Is Prostate Cancer?
Around 20,000 Australian men are diagnosed with prostate cancer each year. It mostly affects men in older age groups and is rare in men under 45 years of age. The chance of developing prostate cancer is significantly higher in men who have a close relative with prostate cancer; the risks are higher if the relative was diagnosed before the age of 60.
Prostate cancer is a disease in which malignant (cancer) cells form in the tissues of the prostate. The prostate is a gland in the male reproductive system located just below the bladder and in front of the rectum.
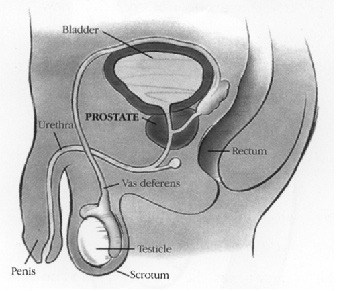
It is about the size of a walnut and surrounds the urethra (the tube that empties urine from the bladder- see picture below). The prostate gland produces fluid that is one of the components of semen.
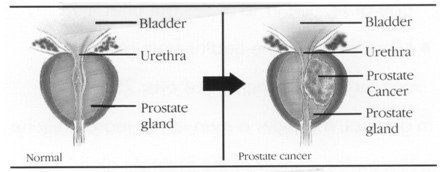
Symptoms and Diagnosis
Urinary symptoms are nonspecific and include
- Frequent urination particularly at night
- Pain on urination
- Blood in the urine
- Weak stream of urine
Prostate cancer can spread to lymph nodes, bones (especially ribs and the hip and lower back), liver and lungs. When the disease spreads to the bones, it causes pain or unexplained weight loss and fatigue.
Digital Rectal Examination (DRE)
Your doctor inserts a gloved finger into the rectum to feel the condition of the prostate that lies close to the rectal wall. If your doctor feels something suspicious such as a lump or bump, further tests will be carried out. Other tests are needed to enable a more accurate diagnosis.
Prostate Specific Antigen (PSA) Test
A blood sample is taken by your doctor to check for prostate specific antigen (PSA), which is produced by the prostate and is increased by cellular abnormalities within the prostate.
As men get older the prostate gland grows and so the PSA is likely to rise. A high PSA may indicate some type of prostate disease. The level can be raised due to inflammation of the prostate (Prostatitis) and enlargement of the prostate gland (Benign Prostatic Hyperplasia or BPH).
PSA is a useful tool for diagnosing and monitoring prostate diseases, but further tests are required to confirm which condition is present.
Trans Rectal Ultrasound Guided biopsies is discussed elsewhere, Click here to find out more.
TRUS BiopsyStaging and Grading
The tests performed are used to determine the stage of the prostate cancer. Biopsy specimens are analysed to find out how aggressive the cancer is.
The staging system describes how far the cancer has spread within and/or beyond the prostate capsule.
Stage 1/A : There are no symptoms and the tumour is confined within the prostate. It is usually found during the investigation of a different complaint.
Stage 2/B : Again the tumour is confined to the prostate and although symptoms may not be apparent, it can be felt during a DRE.
Stage 3/C : The tumour has spread just outside the prostate gland and may effect nearby tissue.
A common symptom is difficulty in urinating.
Stage 4/D : Also known as Metastatic cancer, the tumour has spread to other parts of the body. Bones and Lymph nodes are commonly afflicted and symptoms may include fatigue, weight loss, bone pain and difficulty urinating.
The Gleason Score indicates how aggressive the cancer is. The Gleason Score (or Sum) is the score of aggressiveness of the cancer on careful inspection under the microscope. The Gleason Score is actually made up of 2 numbers known as Gleason Grades. When a pathologist looks at the prostate cancer under the microscope, a number grade from 1 to 5 is assigned to the area most representative of the cancer (the primary Gleason Grade). A second number grade from 1 to 5 is given to the second most representative area within the cancer (the secondary Gleason Grade). These two numbers are added together to give the Gleason score. The maximum Gleason score is 10 and the minimum Gleason score is 2. The higher the score, the more aggressive the tumour is likely to be. This will impact the likely success of treatment.
Bone Scans
Your doctor may want to see if the cancer has metastasised and has affected your bones. A small amount of radioactive material is injected into your arm, which is then absorbed by your bones as they heal. Your arm will then be scanned an hour later to view the activity of the bone and ascertain whether the cancer has spread.